Here we go again. The United States is now experiencing a fourth wave of COVID-19, with very rapidly rising infections. The surge in new daily cases is driven by the Delta variant, which makes up 83% of sequenced samples in the U.S. and which is estimated to be twice as transmissible as the original strain. One of the reasons that Delta spreads more easily is that a person infected with this variant has a viral load 1,000 times higher than someone infected with the original version of SARS-CoV-2.
Hospitalizations and deaths are also rising, though more slowly than cases, reflecting the fact that 49% of all Americans are fully vaccinated. Even with Delta, COVID-19 vaccines are extremely effective at preventing severe illness and death. Anthony Fauci, President Joe Biden’s chief medical advisor on COVID-19, estimates that over 99% of people dying in the U.S. from the illness are unvaccinated. But the levels of vaccination are not high enough in some areas to prevent new surges among those who are not inoculated. And with growing infections among the unvaccinated, some vaccinated people are not surprisingly getting breakthrough infections because no vaccines are 100% effective. So, what happens next? How is the pandemic likely to play out into the fall and winter? Here are six factors that are likely to drive the shape of the pandemic in the coming months.
First, local vaccination rates will continue to be the most important factor in determining what will happen
The U.S. now has a patchwork pandemic, in which communities with low vaccination rates are likeliest to see surges in infection. One recent analysis found that 463 U.S. counties now have high rates of new infection—at least 100 new cases per 100,000 residents in the past week, which is over five times the overall U.S. rate. In 80% of these counties, less than 40% of residents are fully vaccinated. The five states with the lowest rates of full vaccination—Alabama (34%), Arkansas (35%), Louisiana (36%), Mississippi (34%), and Wyoming (36%)—are all experiencing major surges.
In these five states, while 4 out of 5 people aged over 65 have had at least one shot, the vaccination rate is much lower in the 18-65 age group, and lower still in adolescents (those aged 12-17). Few adolescents in these states have had at least one dose: just 24% in Arkansas, 16% in Alabama, 17% in Louisiana, 15% in Mississippi, and 19% in Wyoming. This leaves young people highly vulnerable to the fast-spreading Delta variant. Compare these numbers with a highly vaccinated state like Vermont, where almost 100% of those aged over 65 and 68% of those aged 12-17 have had at least one dose—and cases and hospitalizations are less than 3 and 1 per 100, 000, respectively.
It is also clear that the uptake of vaccines has slowed down and in some places almost stagnated, particularly in the southern states. The U.S. went from administering more than 3 million doses a day in mid-April to only around 500,000 doses a day right now. If you live in a poorly vaccinated community—and especially if vaccination rates are stagnant or barely rising—your community is at an elevated risk of a surge. Data from this week suggest that in some states affected by surges the rate of vaccinations is increasing, but it is unclear if this trend will continue.
In highly vaccinated states, an influx of unvaccinated visitors can also create a potential set up for local outbreaks. We saw this in Provincetown, Mass., where a super-spreader event presumed to be from a large influx of unvaccinated visitors led to a major cluster (430 confirmed cases as of July 23, 2021). Of the Massachusetts residents affected in this outbreak, 69% reported that they were fully vaccinated. And it would have been much worse had the vaccination levels of the Provincetown community not been so high. But the secondary impact of these types of clusters on pockets of unvaccinated children and on high risk or immunocompromised adults will in part depend on the amount of transmission from vaccinated people who have breakthrough infections.
Moving forward, we think a few policy and social aspects will have a huge impact on whether vaccination rates increase in this country—in particular, whether there is a concerted effort to depoliticize vaccines (political affiliation appears to be driving differences in vaccination uptake) and whether more businesses and schools start to require vaccinations for participation and employment.
Second, whether public health measures are reinstated will affect how long those surges continue
In communities facing a surge related to the Delta variant, the right public health response is to restore control measures such as community-wide indoor mask mandates, social distancing rules, scaling up test and trace, and intensifying workplace and school mitigations (including improved ventilation) until vaccination rates increase. Los Angeles county, for example, recently reinstated an indoor mask mandate for everyone, regardless of vaccination status, to help curb its rapid spread of the Delta variant. Similarly, last week San Francisco Bay Area health officials urged residents of seven counties and the city of Berkeley to resume wearing masks indoors. Sound pandemic management requires tailoring measures to the local situation on the ground.
 The U.S. Centers for Disease Control and Prevention (CDC) placed a significant roadblock to such tailored management when it changed its mask guidance in May, saying vaccinated people no longer need to wear masks indoors—this guidance had no nuance to account for community transmission levels or outbreak status. The guidance basically gave local governments and businesses the cover to drop mask mandates and indoor limits for both vaccinated and unvaccinated, leading both to change their behavior and putting other unvaccinated people, including children under 12, at risk. We agree with former Surgeon General Jerome Adams when he says, “the CDC urgently needs to revise its guidance to vaccinate and mask in places where cases are rising yet vaccination rates remain low.” CDC should consider releasing specific metrics for on-ramping and off-ramping public health measures that local and state public health bodies can take into consideration. Such guidance would lead to less confusion and build more public trust. Many schools are reopening in five weeks, and we think there is an urgency for the CDC to provide more specific guidance on masks, testing, and other mitigations against COVID-19 in schools. The American Academy of Pediatrics now recommends that all students over 2 years old, and all teachers and staff, wear masks, regardless of whether they have been vaccinated against COVID-19—that could help, though the need for masking should be tailored to local community transmission levels.
The U.S. Centers for Disease Control and Prevention (CDC) placed a significant roadblock to such tailored management when it changed its mask guidance in May, saying vaccinated people no longer need to wear masks indoors—this guidance had no nuance to account for community transmission levels or outbreak status. The guidance basically gave local governments and businesses the cover to drop mask mandates and indoor limits for both vaccinated and unvaccinated, leading both to change their behavior and putting other unvaccinated people, including children under 12, at risk. We agree with former Surgeon General Jerome Adams when he says, “the CDC urgently needs to revise its guidance to vaccinate and mask in places where cases are rising yet vaccination rates remain low.” CDC should consider releasing specific metrics for on-ramping and off-ramping public health measures that local and state public health bodies can take into consideration. Such guidance would lead to less confusion and build more public trust. Many schools are reopening in five weeks, and we think there is an urgency for the CDC to provide more specific guidance on masks, testing, and other mitigations against COVID-19 in schools. The American Academy of Pediatrics now recommends that all students over 2 years old, and all teachers and staff, wear masks, regardless of whether they have been vaccinated against COVID-19—that could help, though the need for masking should be tailored to local community transmission levels.
University and college campuses will also need to grapple with the challenges that Delta brings. A new study by Yale University researchers David Paltiel and Jason Schwartz found that colleges where over 90% of all students, faculty and staff are fully vaccinated can safely return to normalcy, but campuses below this vaccine coverage may need measures such as distancing and frequent testing of the unvaccinated.
Third, the local pattern of COVID-19 could be influenced by how much protection is provided by past infection.
Research suggests that if you have had COVID-19, you acquire some degree of immunity. In theory this might mean that if your community has low vaccination rates but a high proportion of people were previously infected, the chances of a surge from the Delta variant are lower. But we need to be careful about jumping to any conclusions. The science suggests that the immunity from past infection may be partial and short term, which is why the World Health Organization, CDC, and other public health agencies recommend that people who have been infected by SARS-CoV-2 still get vaccinated. Additionally, a new analysis from Public Health England found that reinfection is more likely with the Delta variant compared to the Alpha variant—further argument for even those who have had and recovered from COVID-19 to get vaccinated.
A fourth factor is whether vulnerable Americans will need booster shots and if some decrease in immunity will lead to seasonal increases in cases, similar to the way influenza rates rise every winter
Last week, Israel’s health ministry released data raising the possibility that the protection that the Pfizer vaccine provides against infection may wane over time. We need to be very cautious about the data: they are preliminary and based on small numbers, and other nations have not seen a similar waning. There are also supportive data based on lab studies that say that for most people, vaccine-induced immunity may last years (at least against the current variants), although such immunity may wane for those who are more advanced in age or have weakened immune systems.
After previously ruling out the need for boosters, the Biden Administration has now signaled that it is looking into recommending a booster (a third shot of either the Pfizer/BioNTech or Moderna vaccine) for people 65 and older or those with weakened immune systems. Experts are also considering whether those who received the single-shot Johnson & Johnson vaccine should get a booster shot of Pfizer/BioNTech or Moderna. At a recent senate hearing, CDC Director Rochelle Walensky said that her agency is following large cohorts of vaccinated residents in nursing homes as well as cohorts of vaccinated frontline health workers with weekly testing to understand how efficacy against vaccines may be changing over time. Such data will likely help determine whether and when boosters are needed.
Some infectious disease experts, such as the German virologist Christian Drosten, believe that COVID-19 could become a “seasonal epidemic,” with an annual rise in cases in the winter. If it turns out that immunity from the vaccine does decline over time among the elderly and immune compromised and that COVID-19 is seasonal, this combination would provide a strong case for giving these vulnerable people boosters ahead of winter.
Fifth, we don’t know exactly how common it is for vaccinated people to become infected and transmit SARS-CoV-2 to others, though so far it appears to be relatively uncommon
The good news is that all the authorized vaccines greatly reduce your chances of becoming infected (e.g. the Pfizer/BioNTech and Moderna vaccines reduce this risk by 91%)—and reduce the risk of becoming severely ill, hospitalized, or dying from COVID-19 at an even higher rate. But no vaccine is 100% effective. So we would still expect a small proportion of fully vaccinated people to get infected and sometimes transmit the virus to others.
Research is underway to try and determine just how common it is for vaccinated people to transmit SARS-CoV-2 to others and how the Delta variant impacts this risk, and the results will have a bearing on the next phase of the pandemic.
Sixth, another new variant of concern could arise
All viruses change (mutate) over time, and such mutations are more likely when a virus is circulating widely. Most mutations don’t change the ability of the virus to cause infections and disease, but some canThat means that, as long as SARS-CoV-2 is spreading, there’s a possibility that new variants of concern could arise, which could again change the trajectory of the pandemic.
The good news is that COVID-19 vaccines are highly effective against all known variants. Scientists are also confident that if a new variant arises that evades the protection of current vaccines, vaccine manufacturers will be able to quickly reformulate and test vaccines against these new variants. But currently, half of America and most parts of the rest of the world are not vaccinated; in Africa, for example, just 2% of people have received at least one dose of the vaccine. Globally, cases and deaths have gone up by 25% over the last two weeks and these continued surges are giving the virus ample opportunity to evolve. As new variants evolve, it won’t be our ability to create reformulated vaccines that will limit us. Instead, the main hurdle will be to turn those new vaccines into vaccinations here in the U.S. and worldwide.
During the 1918 influenza pandemic, one third of the world’s population was infected and society was vulnerable to consecutive waves with minimal number of tools to combat them. In 2021, we have extremely powerful vaccines in addition to tried and true non-pharmaceutical measures such as masks that can help us shape our destinies to a greater measure than was possible a century ago. But the COVID-19 pandemic has revealed that even with these tools, there are significant social and political challenges that are delaying our recovery.

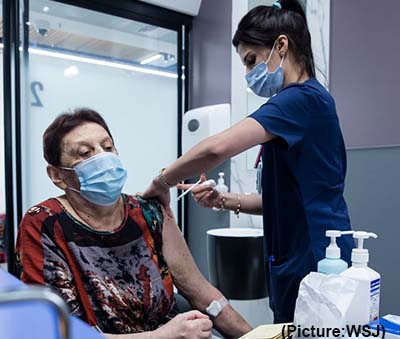 People who tested positive for SARS-CoV-2 after one or two vaccine doses had significantly lower odds of severe disease or hospitalisation than unvaccinated people, according to a large-scale study investigating COVID-19 breakthrough infections published in The Lancet Infectious Diseases journal. Researchers also found that the odds of experiencing long COVID (illness lasting 28 days or more after a positive test) were cut in half for people who received two vaccines doses.
People who tested positive for SARS-CoV-2 after one or two vaccine doses had significantly lower odds of severe disease or hospitalisation than unvaccinated people, according to a large-scale study investigating COVID-19 breakthrough infections published in The Lancet Infectious Diseases journal. Researchers also found that the odds of experiencing long COVID (illness lasting 28 days or more after a positive test) were cut in half for people who received two vaccines doses. The first clue came when the scientists examined images from VLASS, which began observations in 2017, and found an object brightly emitting radio waves but which had not appeared in an earlier VLA sky survey, called Faint Images of the Radio Sky at Twenty centimeters (FIRST). They made subsequent observations of the object, designated VT 1210+4956, using the VLA and the Keck telescope in Hawaii. They determined that the bright radio emission was coming from the outskirts of a dwarf, star-forming galaxy some 480 million light-years from Earth. They later found that an instrument aboard the International Space Station had detected a burst of X-rays coming from the object in 2014.
The first clue came when the scientists examined images from VLASS, which began observations in 2017, and found an object brightly emitting radio waves but which had not appeared in an earlier VLA sky survey, called Faint Images of the Radio Sky at Twenty centimeters (FIRST). They made subsequent observations of the object, designated VT 1210+4956, using the VLA and the Keck telescope in Hawaii. They determined that the bright radio emission was coming from the outskirts of a dwarf, star-forming galaxy some 480 million light-years from Earth. They later found that an instrument aboard the International Space Station had detected a burst of X-rays coming from the object in 2014. A new study has now pointed out that these changes in the Arctic region induced by anthropogenic global warming have disrupted a wind system called Stratospheric Polar Vortex (SPV). This stretching of SPV can lead to extreme cold events in parts of Asia and North America. The report published Friday in Science adds that this SPV disruption was behind the February 2021 Texas cold wave. “The SPV consists of strong westerly winds from 10km to 50km above the surface. It peaks at around 50 m/s on average near 50km and is strongest in mid-winter, however, on occasion it can weaken, and sometimes the winds reverse direction entirely,” explains one of the authors Prof. Chaim Garfinkel in an email to indianexpress.com. He is the Head of the Graduate Program in Atmospheric Science at Hebrew University, Israel. He adds that these stretching events almost certainly occurred before greenhouse gas emissions began increasing, but the current emissions are leading to an increase in the occurrence of these types of events.
A new study has now pointed out that these changes in the Arctic region induced by anthropogenic global warming have disrupted a wind system called Stratospheric Polar Vortex (SPV). This stretching of SPV can lead to extreme cold events in parts of Asia and North America. The report published Friday in Science adds that this SPV disruption was behind the February 2021 Texas cold wave. “The SPV consists of strong westerly winds from 10km to 50km above the surface. It peaks at around 50 m/s on average near 50km and is strongest in mid-winter, however, on occasion it can weaken, and sometimes the winds reverse direction entirely,” explains one of the authors Prof. Chaim Garfinkel in an email to indianexpress.com. He is the Head of the Graduate Program in Atmospheric Science at Hebrew University, Israel. He adds that these stretching events almost certainly occurred before greenhouse gas emissions began increasing, but the current emissions are leading to an increase in the occurrence of these types of events. Affiliated with various US medical organizations and institutions, the soft-spoken Dr. Murthy is a Resuscitation Educator and Researcher, Advisor to Resuscitation Training Centers, Champion of Community Cardiopulmonary Resuscitation (CPR), and a Leader of US Organized Medicine. His Mission has been “Saving Lives” in Sudden Cardiac Arrests and common heart issues.
Affiliated with various US medical organizations and institutions, the soft-spoken Dr. Murthy is a Resuscitation Educator and Researcher, Advisor to Resuscitation Training Centers, Champion of Community Cardiopulmonary Resuscitation (CPR), and a Leader of US Organized Medicine. His Mission has been “Saving Lives” in Sudden Cardiac Arrests and common heart issues. The Founder of Chicago Medical Society’s Community CPR Project Saving More Illinois Lives through Education (SMILE,) Dr. Murthy, takes upon himself the life-long mission of saving lives through effective preventive measures. He says, “Almost one in three among South Asians may die from heart disease before 65 years of age.”
The Founder of Chicago Medical Society’s Community CPR Project Saving More Illinois Lives through Education (SMILE,) Dr. Murthy, takes upon himself the life-long mission of saving lives through effective preventive measures. He says, “Almost one in three among South Asians may die from heart disease before 65 years of age.” Dr. Murthy served the American Heart Association in different capacities. Such as National and International Faculty, Member of the International Committee, and Advisor to AHA International Training Centers, Also as AHA Liaison to Medical Organizations in the USA too. He co-chaired programs at the AHA Scientific Sessions and delivered Resuscitation-based lectures at prestigious US medical institutions.
Dr. Murthy served the American Heart Association in different capacities. Such as National and International Faculty, Member of the International Committee, and Advisor to AHA International Training Centers, Also as AHA Liaison to Medical Organizations in the USA too. He co-chaired programs at the AHA Scientific Sessions and delivered Resuscitation-based lectures at prestigious US medical institutions. U.S. Surgeon General Dr. Vivek Murthy has defended the Biden administration’s plans to
U.S. Surgeon General Dr. Vivek Murthy has defended the Biden administration’s plans to  Chaired by Prime Minister Narendra Modi, the Cabinet gave its approval for signing the MoU between the GSI, under the Ministry of Mines, and the varsity’s board of trustees on behalf of its Department of Earth and Environment, a government statement said. The identified area of cooperation between the two participants would include development of geological knowledge, research regarding geologic and tectonic environment of post collisions magmatism in India-Asia collisional margin, geologic history and tectonics of the Eastern Himalayan Syntaxis and developing cooperative projects in the fields of regional geological, geochemical, petrological and multi-isotopic studies related to the evolution of post collisional magmatic belts.
Chaired by Prime Minister Narendra Modi, the Cabinet gave its approval for signing the MoU between the GSI, under the Ministry of Mines, and the varsity’s board of trustees on behalf of its Department of Earth and Environment, a government statement said. The identified area of cooperation between the two participants would include development of geological knowledge, research regarding geologic and tectonic environment of post collisions magmatism in India-Asia collisional margin, geologic history and tectonics of the Eastern Himalayan Syntaxis and developing cooperative projects in the fields of regional geological, geochemical, petrological and multi-isotopic studies related to the evolution of post collisional magmatic belts. “FOOD WITHOUT FEAR: Identify, Prevent, and Treat Food Allergies, Intolerances, and Sensitivities,” a newly released book by Dr. Ruchi Gupta, an young and talented Indian American, illuminates what she has coined the food reaction spectrum—a revolutionary way to look at food-related conditions—and offers a new approach to managing adverse responses to food with a practical plan to end the misery and enjoy eating with ease.
“FOOD WITHOUT FEAR: Identify, Prevent, and Treat Food Allergies, Intolerances, and Sensitivities,” a newly released book by Dr. Ruchi Gupta, an young and talented Indian American, illuminates what she has coined the food reaction spectrum—a revolutionary way to look at food-related conditions—and offers a new approach to managing adverse responses to food with a practical plan to end the misery and enjoy eating with ease. Dr. Gupta is world-renowned for her groundbreaking research in the areas of food allergy and asthma epidemiology, most notably for her research on the prevalence of pediatric and adult food allergy in the United States. She has also significantly contributed to academic research in the areas of food allergy prevention, socioeconomic disparities in care, and the daily management of these conditions. Dr. Gupta is the author of The Food Allergy Experience, has written and co-authored over 150 peer-reviewed research manuscripts, and has had her work featured on major TV networks and in print media.
Dr. Gupta is world-renowned for her groundbreaking research in the areas of food allergy and asthma epidemiology, most notably for her research on the prevalence of pediatric and adult food allergy in the United States. She has also significantly contributed to academic research in the areas of food allergy prevention, socioeconomic disparities in care, and the daily management of these conditions. Dr. Gupta is the author of The Food Allergy Experience, has written and co-authored over 150 peer-reviewed research manuscripts, and has had her work featured on major TV networks and in print media. “If there was still a need for a proof that climate changes is caused by human activities, then this is the report that provides it,” said Prof Corinne Le Quéré of the University of East Anglia. And the consequences of humanity’s massive act of atmospheric interference are now clear: what is hot today will become hotter tomorrow; extreme floods will become more frequent, wildfires more dangerous and deadly droughts more widespread. In short,
“If there was still a need for a proof that climate changes is caused by human activities, then this is the report that provides it,” said Prof Corinne Le Quéré of the University of East Anglia. And the consequences of humanity’s massive act of atmospheric interference are now clear: what is hot today will become hotter tomorrow; extreme floods will become more frequent, wildfires more dangerous and deadly droughts more widespread. In short,  The Atlantic Meridional Overturning Circulation (AMOC) — which the Gulf Stream is a major part of — helps maintain the energy balance in the Atlantic Ocean. It is often described as a “conveyor belt” that takes warm surface water from the tropics and distributes it to the north Atlantic. The colder, saltier water then sinks and flows south.
The Atlantic Meridional Overturning Circulation (AMOC) — which the Gulf Stream is a major part of — helps maintain the energy balance in the Atlantic Ocean. It is often described as a “conveyor belt” that takes warm surface water from the tropics and distributes it to the north Atlantic. The colder, saltier water then sinks and flows south. This scenario was the premise for the 2004 climate science fiction film “The Day After Tomorrow,” in which a series of extreme weather disasters strike after climate change caused the AMOC to collapse.
This scenario was the premise for the 2004 climate science fiction film “The Day After Tomorrow,” in which a series of extreme weather disasters strike after climate change caused the AMOC to collapse. Between 40 and 34 million years ago, Earth’s climate underwent a major climatic transition. Before 40 million years ago, during the Eocene, Antarctica was covered by lush forests, but by 34 million years ago, in the Oligocene, these forests had been replaced by thick continental ice sheets, as we know Antarctica today. The main driver of this greenhouse to icehouse transition is widely debated, and little information is available about how climate changed on land. An international team led by Dr Vittoria Lauretano and
Between 40 and 34 million years ago, Earth’s climate underwent a major climatic transition. Before 40 million years ago, during the Eocene, Antarctica was covered by lush forests, but by 34 million years ago, in the Oligocene, these forests had been replaced by thick continental ice sheets, as we know Antarctica today. The main driver of this greenhouse to icehouse transition is widely debated, and little information is available about how climate changed on land. An international team led by Dr Vittoria Lauretano and  “We recognize that for some, the FDA approval of COVID-19 vaccines may bring additional confidence and encourage them to get vaccinated,” Abigail Capobianco, a spokeswoman at the FDA, said in a statement on Aug. 4. “Acknowledging the urgency related to the current state of the pandemic, we have taken an all-hands-on-deck approach, including identifying additional resources such as personnel and technological resources from across the agency and opportunities to reprioritize other activities, in order to complete our review to help combat this pandemic surge.”
“We recognize that for some, the FDA approval of COVID-19 vaccines may bring additional confidence and encourage them to get vaccinated,” Abigail Capobianco, a spokeswoman at the FDA, said in a statement on Aug. 4. “Acknowledging the urgency related to the current state of the pandemic, we have taken an all-hands-on-deck approach, including identifying additional resources such as personnel and technological resources from across the agency and opportunities to reprioritize other activities, in order to complete our review to help combat this pandemic surge.” The agency said the halt should last at least two months, to give the world a chance to meet the director-general’s goal of vaccinating 10% of the population of every country by the end of September.
The agency said the halt should last at least two months, to give the world a chance to meet the director-general’s goal of vaccinating 10% of the population of every country by the end of September. Ram N Kumar, the founder of NirogStreet, has told the media that he was fortunate to find a clutch of investors from the US, who could not just invest but guide. “For me, if you get a person like Gokul to help you while building a company, it is a once in a lifetime opportunity,” Kumar said.
Ram N Kumar, the founder of NirogStreet, has told the media that he was fortunate to find a clutch of investors from the US, who could not just invest but guide. “For me, if you get a person like Gokul to help you while building a company, it is a once in a lifetime opportunity,” Kumar said. When a person is infected with COVID-19, antibodies are typically produced to fight against the invading disease. These antibodies are unique to each individual, meaning that some antibodies are better than others at combating the virus. Thus, pharmaceutical companies study thousands of these antibodies to take advantage of the most effective ones with the highest barrier to resistance.
When a person is infected with COVID-19, antibodies are typically produced to fight against the invading disease. These antibodies are unique to each individual, meaning that some antibodies are better than others at combating the virus. Thus, pharmaceutical companies study thousands of these antibodies to take advantage of the most effective ones with the highest barrier to resistance. Ashwagandha (Withania Somnifera), commonly known as ‘Indian winter cherry’, is a traditional Indian herb that boosts energy, reduces stress, and makes the immune system stronger.
Ashwagandha (Withania Somnifera), commonly known as ‘Indian winter cherry’, is a traditional Indian herb that boosts energy, reduces stress, and makes the immune system stronger. It’s not just our memories — this past June was the hottest June recorded in the U.S. in more than a century, about four degrees hotter on average. Heat waves (like in the
It’s not just our memories — this past June was the hottest June recorded in the U.S. in more than a century, about four degrees hotter on average. Heat waves (like in the  The U.S. Centers for Disease Control and Prevention (CDC) placed a significant roadblock to such tailored management when it changed its
The U.S. Centers for Disease Control and Prevention (CDC) placed a significant roadblock to such tailored management when it changed its A full course of two of the most widely available coronavirus vaccines is about as effective against the more contagious delta variant as it was against a previously dominant version of the virus, according to
A full course of two of the most widely available coronavirus vaccines is about as effective against the more contagious delta variant as it was against a previously dominant version of the virus, according to  As a result, researchers expected another coronavirus epidemic or pandemic, though not necessarily one as bad as the COVID-19 outbreak. “This was the worst by far,” he said. Researchers anticipated the initial outbreak from China where the preceding epidemics occurred, but were surprised it came from Central China, not Southern China, as was the case with the 2002 SARS epidemic, he said.
As a result, researchers expected another coronavirus epidemic or pandemic, though not necessarily one as bad as the COVID-19 outbreak. “This was the worst by far,” he said. Researchers anticipated the initial outbreak from China where the preceding epidemics occurred, but were surprised it came from Central China, not Southern China, as was the case with the 2002 SARS epidemic, he said. Bernardinelli and Bernstein used algorithms at the National Center for Supercomputing Applications at the University of Illinois at Urbana-Champaign to identify trans-Neptunian objects. During their work, the astronomers traced 32 detections to one object. Comets are icy relics that were kicked out of the solar system when the giant planets formed and migrated to their current configurations. As comets approach our sun during their orbits, their ices evaporate, creating their signature appearance.
Bernardinelli and Bernstein used algorithms at the National Center for Supercomputing Applications at the University of Illinois at Urbana-Champaign to identify trans-Neptunian objects. During their work, the astronomers traced 32 detections to one object. Comets are icy relics that were kicked out of the solar system when the giant planets formed and migrated to their current configurations. As comets approach our sun during their orbits, their ices evaporate, creating their signature appearance. Each yearly delineation on the sequoia’s surface is a small part of a far grander story that ties together all of life on Earth. Scientists know this as Deep Time. It’s not just on the scale of centuries, millennia, epochs, or periods, but the ongoing flow that goes back to the origins of our universe, the formation of the Earth, and the evolution of all life, up through this present moment. It’s the backdrop for everything we see around us today, and it can be understood through techniques as different as absolute dating of radioactive minerals and counting the rings of a prehistoric tree. Each part informs the whole.
Each yearly delineation on the sequoia’s surface is a small part of a far grander story that ties together all of life on Earth. Scientists know this as Deep Time. It’s not just on the scale of centuries, millennia, epochs, or periods, but the ongoing flow that goes back to the origins of our universe, the formation of the Earth, and the evolution of all life, up through this present moment. It’s the backdrop for everything we see around us today, and it can be understood through techniques as different as absolute dating of radioactive minerals and counting the rings of a prehistoric tree. Each part informs the whole. The co-axial electrospinning technique is one of the most favorable and simple options to fabricate membranes with three-dimensional hierarchical structures. Dr. Woo’s research team used poly(vinylidene fluoride-co-hexafluoropropylene) as the core and silica aerogel mixed with a low concentration of the polymer as the sheath to produce a co-axial composite membrane and obtain a superhydrophobic membrane surface. In fact, silica aerogel exhibited a much lower thermal conductivity compared with that of conventional polymers, which led to increased water vapor flux during the membrane distillation process due to a reduction of conductive heat losses.
The co-axial electrospinning technique is one of the most favorable and simple options to fabricate membranes with three-dimensional hierarchical structures. Dr. Woo’s research team used poly(vinylidene fluoride-co-hexafluoropropylene) as the core and silica aerogel mixed with a low concentration of the polymer as the sheath to produce a co-axial composite membrane and obtain a superhydrophobic membrane surface. In fact, silica aerogel exhibited a much lower thermal conductivity compared with that of conventional polymers, which led to increased water vapor flux during the membrane distillation process due to a reduction of conductive heat losses. France, Germany and Italy, among other countries, now advise only one dose of vaccine for people with a healthy immune system and a confirmed previous diagnosis. Many scientists who have studied immune responses to vaccination say such policies are a sensible way to make the most of
France, Germany and Italy, among other countries, now advise only one dose of vaccine for people with a healthy immune system and a confirmed previous diagnosis. Many scientists who have studied immune responses to vaccination say such policies are a sensible way to make the most of  Over the centuries, the June solstice has inspired countless festivals,
Over the centuries, the June solstice has inspired countless festivals,  Co-authored by research scientists and engineers from WHOI, MBARI (Monterey Bay Aquarium Research Institute), and Stanford University, the paper outlines the robot’s success in autonomously tracking two gelatinous marine creatures during a 2019 research cruise in Monterey Bay. High-definition video revealed a “dinner plate” jellyfish “ramming” a siphonophore, which narrowly escaped the jelly’s venomous tentacles. Mesobot also recorded a 30-minute video of a giant larvacean, which appears to be nearly motionless but is actually riding internal waves that rise and fall 6 meters (20 feet). These observations represent the first time that a self-guided robot has tracked these small, clear creatures as they move through the water column like a “parcel of water,” said Yoerger.
Co-authored by research scientists and engineers from WHOI, MBARI (Monterey Bay Aquarium Research Institute), and Stanford University, the paper outlines the robot’s success in autonomously tracking two gelatinous marine creatures during a 2019 research cruise in Monterey Bay. High-definition video revealed a “dinner plate” jellyfish “ramming” a siphonophore, which narrowly escaped the jelly’s venomous tentacles. Mesobot also recorded a 30-minute video of a giant larvacean, which appears to be nearly motionless but is actually riding internal waves that rise and fall 6 meters (20 feet). These observations represent the first time that a self-guided robot has tracked these small, clear creatures as they move through the water column like a “parcel of water,” said Yoerger. NASA states that the NGC 4680 is a tricky galaxy to classify. The space agency further states that this is because the galaxy is sometimes referred to as a spiral galaxy, but it is also sometimes classified as a lenticular galaxy. Lenticular galaxies are said to fall somewhere in between spiral galaxies and elliptical galaxies. The NGC 4680 galaxy is said to have distinguishable spiral arms that are not clearly defined, and the tip of one arm appears very diffuse.
NASA states that the NGC 4680 is a tricky galaxy to classify. The space agency further states that this is because the galaxy is sometimes referred to as a spiral galaxy, but it is also sometimes classified as a lenticular galaxy. Lenticular galaxies are said to fall somewhere in between spiral galaxies and elliptical galaxies. The NGC 4680 galaxy is said to have distinguishable spiral arms that are not clearly defined, and the tip of one arm appears very diffuse. In March 2019, late-stage international trials of aducanumab, involving about 3,000 patients, were halted when analysis showed the drug, given as a monthly infusion, was not better at slowing the deterioration of memory and thinking problems than a dummy drug.But later that year, the US manufacturer Biogen analysed more data and concluded the drug did work, as long as it was given in higher doses. The company also said it significantly slowed cognitive decline.Aducanumab targets amyloid, a protein that forms abnormal clumps in the brains of people with Alzheimer’s that can damage cells and trigger dementia, including:
In March 2019, late-stage international trials of aducanumab, involving about 3,000 patients, were halted when analysis showed the drug, given as a monthly infusion, was not better at slowing the deterioration of memory and thinking problems than a dummy drug.But later that year, the US manufacturer Biogen analysed more data and concluded the drug did work, as long as it was given in higher doses. The company also said it significantly slowed cognitive decline.Aducanumab targets amyloid, a protein that forms abnormal clumps in the brains of people with Alzheimer’s that can damage cells and trigger dementia, including: This idea of electrons “surfing” on the electric field is a theory first introduced in 1946 by a Russian physicist, Lev Landau, that was named Landau damping. His theory has now been proven.Recreating the northern lights Scientists have understood for decades how the aurora most likely is created, but they have now been able to simulate it, for the first time, in a lab at the Large Plasma Device (LPD) in UCLA’s Basic Plasma Science Facility.Scientists used a 20-meter-long chamber to recreate Earth’s magnetic field using the powerful magnetic field coils on UCLA’s LPD. Inside the chamber, scientists generated a plasma similar to what exists in space near the Earth.
This idea of electrons “surfing” on the electric field is a theory first introduced in 1946 by a Russian physicist, Lev Landau, that was named Landau damping. His theory has now been proven.Recreating the northern lights Scientists have understood for decades how the aurora most likely is created, but they have now been able to simulate it, for the first time, in a lab at the Large Plasma Device (LPD) in UCLA’s Basic Plasma Science Facility.Scientists used a 20-meter-long chamber to recreate Earth’s magnetic field using the powerful magnetic field coils on UCLA’s LPD. Inside the chamber, scientists generated a plasma similar to what exists in space near the Earth. In 2020 – one of the three warmest years on record – the global average temperature was 1.2 degrees Celsius above the pre-industrial baseline, according to an April
In 2020 – one of the three warmest years on record – the global average temperature was 1.2 degrees Celsius above the pre-industrial baseline, according to an April  Dr. Susan R. Bailey, President of American Medication Association (AMA), who was the Chief Guest and Distinguished speaker at the launch event, inaugurated JAAPI on Wednesday, May 12, 2021 during a solemn virtual ceremony, attended by hundreds of AAPI members and supporters from around the nation.Dr. Susan R. Bailey, while inaugurating JAAPI said, “It’s my pleasure to celebrate the launch of JAAPI. On behalf of AMA we congratulate AAPI for this new initiative, which will be a great source of medical education. We applaud you and looking forward to reading your great contributions in the years to come.”
Dr. Susan R. Bailey, President of American Medication Association (AMA), who was the Chief Guest and Distinguished speaker at the launch event, inaugurated JAAPI on Wednesday, May 12, 2021 during a solemn virtual ceremony, attended by hundreds of AAPI members and supporters from around the nation.Dr. Susan R. Bailey, while inaugurating JAAPI said, “It’s my pleasure to celebrate the launch of JAAPI. On behalf of AMA we congratulate AAPI for this new initiative, which will be a great source of medical education. We applaud you and looking forward to reading your great contributions in the years to come.” “Physician Leadership In Times of Crisis & Transition” was the theme of an hour long CME presented by Dr. Bailey at the conclusion of the JAAPI launch ceremony. The insightful and practically oriented CME was organized by American Association of Physicians of Indian Origin, in affiliation with Chicago Medical Society and in association with Indian American Medical Association of Illinois IAMA (IL.)
“Physician Leadership In Times of Crisis & Transition” was the theme of an hour long CME presented by Dr. Bailey at the conclusion of the JAAPI launch ceremony. The insightful and practically oriented CME was organized by American Association of Physicians of Indian Origin, in affiliation with Chicago Medical Society and in association with Indian American Medical Association of Illinois IAMA (IL.) The findings showed that the chance of death rose between 2016 and 2018 by 7 per cent in hospitals that did not implement the policy, and fell by 11 per cent in hospitals that did implement the policy.The chances of being re-admitted increased by 6 per cent in the comparison hospitals over time, but stayed the same in hospitals that implemented the policy. Between 2016 and 2018, the length of stay fell by 5 per cent in the hospitals that did not implement the policy, and by 9 per cent in hospitals that did.
The findings showed that the chance of death rose between 2016 and 2018 by 7 per cent in hospitals that did not implement the policy, and fell by 11 per cent in hospitals that did implement the policy.The chances of being re-admitted increased by 6 per cent in the comparison hospitals over time, but stayed the same in hospitals that implemented the policy. Between 2016 and 2018, the length of stay fell by 5 per cent in the hospitals that did not implement the policy, and by 9 per cent in hospitals that did. Dexamethasone, an inexpensive corticosteroid, is an older drug that has been found most beneficial in hospitalized patients who require invasive mechanical ventilation. Yet, when given too early in Covid-19, for example, when supplemental oxygen is not required, dexamethasone may be detrimental. Dexamethasone may also be inappropriate for use in patients that have co-morbidities such as obesity and diabetes. Dexamethasone has been used to reduce cellular immune responses and treat patients with acute respiratory distress syndrome (ARDS). It is now repurposed to combat severe symptoms of Covid-19 and is one tool in the Covid-19 treatment armamentarium.
Dexamethasone, an inexpensive corticosteroid, is an older drug that has been found most beneficial in hospitalized patients who require invasive mechanical ventilation. Yet, when given too early in Covid-19, for example, when supplemental oxygen is not required, dexamethasone may be detrimental. Dexamethasone may also be inappropriate for use in patients that have co-morbidities such as obesity and diabetes. Dexamethasone has been used to reduce cellular immune responses and treat patients with acute respiratory distress syndrome (ARDS). It is now repurposed to combat severe symptoms of Covid-19 and is one tool in the Covid-19 treatment armamentarium. “The changes in NOAA’s new report are only a degree or less but can still have a big impact, especially when much of the past century has seen steadily increasing temperatures, with the most pronounced changes occurring in the past several decades,” said Nick Bassill, a meteorologist at the University at Albany. “The unfortunate thing is that this does not make a bigger splash, even though it’s almost universally accepted that the new climate normals were going to come in warmer than the last report.”
“The changes in NOAA’s new report are only a degree or less but can still have a big impact, especially when much of the past century has seen steadily increasing temperatures, with the most pronounced changes occurring in the past several decades,” said Nick Bassill, a meteorologist at the University at Albany. “The unfortunate thing is that this does not make a bigger splash, even though it’s almost universally accepted that the new climate normals were going to come in warmer than the last report.” On query of Professor Medvedev that what value the study of ‘thukdam’ could have for humanity in general. The spiritual leader replied Tibetan Buddhists believe that people go through a process of dissolution in the course of death.
On query of Professor Medvedev that what value the study of ‘thukdam’ could have for humanity in general. The spiritual leader replied Tibetan Buddhists believe that people go through a process of dissolution in the course of death. ASEI Michigan chapter president Muthu Sivanantham introduced and facilitated discussion with the next two speakers. Dr Raj Ramesh, a TEDx speaker who happens to have a doctorate in AI was the next author to speak. He has broad experience with digital transformation and helps organizations bring together complementary strengths of machines and humans to effect grand change. His talk featuring interesting doodles and interactive audience participation surveys was patterned on his recent book, “AI & You” and he advised how to co-exist with machines by sharing how to think, thrive, and transform in an AI driven future.
ASEI Michigan chapter president Muthu Sivanantham introduced and facilitated discussion with the next two speakers. Dr Raj Ramesh, a TEDx speaker who happens to have a doctorate in AI was the next author to speak. He has broad experience with digital transformation and helps organizations bring together complementary strengths of machines and humans to effect grand change. His talk featuring interesting doodles and interactive audience participation surveys was patterned on his recent book, “AI & You” and he advised how to co-exist with machines by sharing how to think, thrive, and transform in an AI driven future. United States Special Presidential Envoy for Climate, John Kerry had met Prime Minister Narendra Modi and environment minister Prakash Javadekar earlier this month regarding increasing climate ambition ahead of COP 26 in Glasgow this November. Minister for Europe and Foreign Affairs of France, Jean-Yves Le Drian had also met Javadekar and said all countries should be on track to achieve carbon neutrality and start phasing out coal.
United States Special Presidential Envoy for Climate, John Kerry had met Prime Minister Narendra Modi and environment minister Prakash Javadekar earlier this month regarding increasing climate ambition ahead of COP 26 in Glasgow this November. Minister for Europe and Foreign Affairs of France, Jean-Yves Le Drian had also met Javadekar and said all countries should be on track to achieve carbon neutrality and start phasing out coal. After one day, the researchers reported, they were able to detect human cells growing in 132 of the embryos and were able study the embryos for up to 19 days. That enabled the scientists to learn more about how animal cells and human cells communicate, an important step toward eventually helping researchers find new ways to grow organs for transplantation in other animals, Belmonte said.
After one day, the researchers reported, they were able to detect human cells growing in 132 of the embryos and were able study the embryos for up to 19 days. That enabled the scientists to learn more about how animal cells and human cells communicate, an important step toward eventually helping researchers find new ways to grow organs for transplantation in other animals, Belmonte said. Archaeologists started excavating in September in the area between the temples of King Ramses III and Amenhotep III. The original goal of the mission was to find King Tutankhamen’s mortuary temple, the statement said.
Archaeologists started excavating in September in the area between the temples of King Ramses III and Amenhotep III. The original goal of the mission was to find King Tutankhamen’s mortuary temple, the statement said.