How Lifestyle Medicine Is Redefining Modern Health: A preventive approach to chronic disease is gaining global attention
By Dr. Anupama Gotimukula, MD, Dip ABLM – Board-Certified Lifestyle Medicine Specialist & Pediatric Anesthesiologist
“Our bodies constantly communicate with us. When we ignore sleep deprivation, stress, diet, physical inactivity, and indulge in recreational habits like smoking & alcohol, disease becomes the body’s way of forcing attention.” – Dr. Anupama Gotimukula
Listening to the Body Before Disease Speaks
Modern medicine has achieved extraordinary advances in treating illness, yet chronic diseases continue to rise worldwide. Health experts now emphasize a powerful but often overlooked truth: many diseases begin long before symptoms appear.
Our bodies constantly communicate with us. When we ignore sleep deprivation, stress, diet, physical inactivity, and indulge in recreational habits like smoking & alcohol, disease becomes the body’s way of forcing attention. – Dr. Anupama Gotimukula
Lifestyle Medicine — an evidence-based medical specialty — focuses on identifying and correcting the root causes of disease rather than managing disease symptoms alone. A preventive approach to chronic disease is gaining global attention!
America’s Chronic Disease Crisis
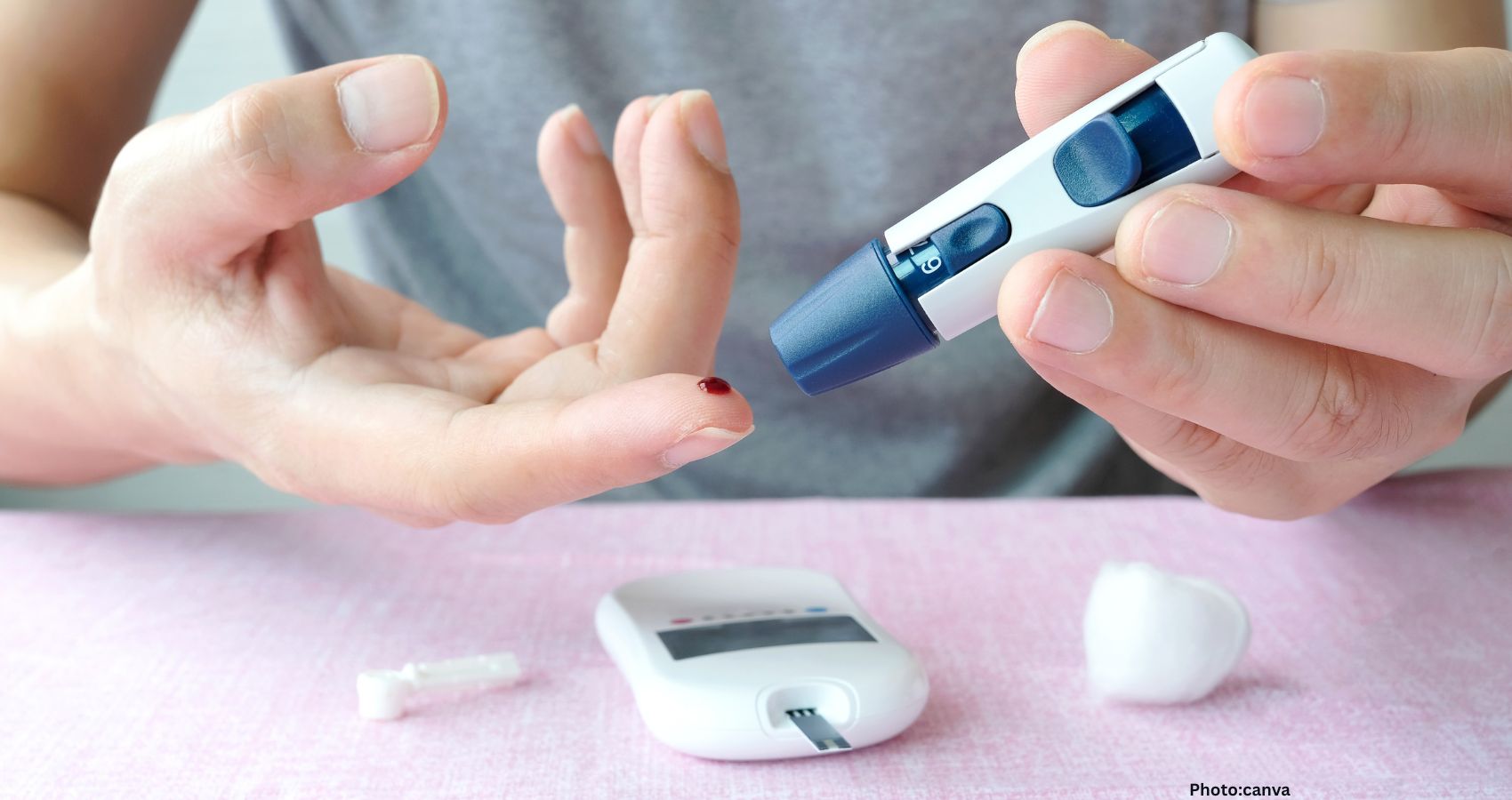
Chronic diseases like high blood pressure, diabetes, heart disease, and obesity are now the leading causes of illness and healthcare costs in the United States. Six in ten American adults live with at least one chronic disease, and four in ten have two or more, which affects quality of life, work, family, and financial stability. Countries like India and many other countries adopting westernized lifestyles are experiencing similar health trends, signaling a global public health challenge.
From Treatment to Prevention: A Medical Shift
Major medical organizations, including the American College of Cardiology, American Heart Association, American Medical Association, and many other organizations, are increasingly emphasizing lifestyle interventions as foundational healthcare, not as a secondary support.
New prevention guidelines now recommend earlier screening and lifestyle interventions beginning around age 30 — reflecting a systemic shift toward preventive medicine.
What are the root causes of Disease? And Why Lifestyle Medicine Matters?
Root causes of disease are the unhealthy lifestyle habits- poor diet, eating more processed & ultra-processed foods, sedentary lifestyle, chronic stress, poor sleep habits, social loneliness, smoking & chronic alcohol use. Lifestyle Medicine is an evidence-based medical specialty that focuses on finding and treating the root causes ![]() of disease rather than only managing disease with medications and procedures. Research shows that intensive lifestyle changes can put conditions like type 2 diabetes into remission in many people and reduce the need for medications. When these areas are addressed together, they can prevent disease, slow or even reverse its progression, and help people feel better physically and mentally at every age.
of disease rather than only managing disease with medications and procedures. Research shows that intensive lifestyle changes can put conditions like type 2 diabetes into remission in many people and reduce the need for medications. When these areas are addressed together, they can prevent disease, slow or even reverse its progression, and help people feel better physically and mentally at every age.
![]() Chronic Disease in U.S. Adults:
Chronic Disease in U.S. Adults:
Most adults now live with at least one or two chronic conditions, but many of these are influenced by daily habits.
What Is Lifestyle Medicine?
![]() Lifestyle Medicine uses scientifically validated evidence-based behavioral and therapeutic interventions organized into six core pillars:
Lifestyle Medicine uses scientifically validated evidence-based behavioral and therapeutic interventions organized into six core pillars:
· Whole-food, plant-predominant nutrition
· Regular physical activity
· Restorative sleep
· Stress management
· Avoidance of risky substances
· Positive social connections
![]() Lifestyle Medicine (LM) places the patient, not the medications or procedural treatments, at the center, in contrast to allopathic medicine. LM integrates multiple disciplines such as nutrition science, positive Psychology, behavior change, exercise physiology, sleep medicine, and addiction medicine, and is very affordable. Teaching self-care and self-management are important elements of lifestyle medicine.
Lifestyle Medicine (LM) places the patient, not the medications or procedural treatments, at the center, in contrast to allopathic medicine. LM integrates multiple disciplines such as nutrition science, positive Psychology, behavior change, exercise physiology, sleep medicine, and addiction medicine, and is very affordable. Teaching self-care and self-management are important elements of lifestyle medicine.
The goals of disease prevention and management are summarized as RRR:
· Root cause of disease
· Remission of disease
· Reversal of disease
Let’s review the 6 core pillars of Lifestyle Medicine
Pillar 1 – Food as Daily Medicine
What we eat every day can either protect our brain, heart, and metabolism—or slowly damage them. Lifestyle Medicine encourages a whole-food, plant-predominant way of eating—centered on vegetables, fruits, whole grains, beans, lentils, nuts, and seeds—with limited processed meat, added sugars, and fast food. Processed foods are altered from their natural form by adding sugar, salt, unhealthy fats, and additives; ultra-processed foods go even further and are highly engineered, convenient, and often addictive. High intake of ultra-processed foods is linked with inflammation, weight gain, worse brain health, and an increased risk of stroke and cognitive decline.
Diets such as the Mediterranean, DASH, and MIND patterns are associated with lower blood pressure, better blood sugar control, and slower brain aging. For example, the DASH diet has been shown to reduce systolic blood pressure by about 8–14 mm Hg in many people, which can significantly lower stroke and heart disease risk.
![]() Practical “Plate” Tips for Readers
Practical “Plate” Tips for Readers
· Fill half your plate with colorful vegetables at lunch and dinner.
· Choose whole grains such as brown rice, oats, or whole-wheat bread instead of refined white versions.
· Make plant proteins (beans, lentils, tofu, nuts) a regular part of meals.
· Replace sugary drinks with water, sparkling water, or unsweetened tea.
· Limit processed meats and deep-fried foods to occasional treats, not daily staples.
For weight management, many adults benefit from tracking calorie intake (for example, 1,200–1,800 calories per day depending on age, sex, and activity) using apps such as MyFitnessPal or similar calorie trackers. The goal is to eat in a way that feels sustainable, affordable, and enjoyable, not like a short-term “crash diet.”
![]() Diet Pattern vs Disease Risk
Diet Pattern vs Disease Risk
Better diet patterns are consistently linked with lower risk of heart disease, diabetes, and cognitive decline.
Pillar 2 – Movement: “Exercise Is Medicine”
Physical inactivity is now considered one of the major preventable causes of illness and early death worldwide. Nearly 80% of Americans do not meet recommended physical activity guidelines, which increases the risk of heart disease, diabetes, some cancers, and depression.
Even simple movement, such as regular walking, can have powerful effects. Studies show that people who reach around 10,000 steps per day often have a substantially lower risk of death compared with those who are highly sedentary, though benefits begin to appear well before that point. Activity improves blood sugar control, blood pressure, mood, stress hormones, and brain health.
Practical Weekly Targets
· ![]() Aim for 150–300 minutes of moderate aerobic activity (such as brisk walking) each week, which is about 30–45 minutes on most days.
Aim for 150–300 minutes of moderate aerobic activity (such as brisk walking) each week, which is about 30–45 minutes on most days.
· Add strength training (using body weight, resistance bands, or weights) at least two days per week for muscle and bone health.
· Include flexibility and balance work—such as yoga or tai chi—to reduce falls and improve body awareness.
Every extra 2,000–3,000 steps per day can make a meaningful difference for long-term health.
Pillar 3 – Sleep: The Forgotten Superpower
![]() The National Sleep Foundation recommends 7–9 hours of quality sleep for most adults, yet at least one-third of adults routinely sleep less than that. Short or poor-quality sleep raises the risk of heart disease, diabetes, obesity, depression, anxiety, and weakened immune function.
The National Sleep Foundation recommends 7–9 hours of quality sleep for most adults, yet at least one-third of adults routinely sleep less than that. Short or poor-quality sleep raises the risk of heart disease, diabetes, obesity, depression, anxiety, and weakened immune function.
Common sleep disruptors include late-day caffeine, screen time and bright light at night, an irregular schedule, and lack of daytime physical activity. Lifestyle Medicine prioritizes non-drug approaches first, such as cognitive behavioral therapy for insomnia and “sleep hygiene” habits, before turning to sleeping pills.
Reader-Friendly Sleep Habits
· Keep a regular sleep and wake time, even on weekends.
· Limit screens and bright light for 1 hour before bed; consider a relaxing routine like reading or gentle stretching.
· Avoid caffeine in the late afternoon and evening.
Pillar 4 – Calming Stress and Protecting the Mind
![]() Chronic stress activates the body’s “fight or flight” system, raising levels of stress hormones like cortisol and, over time, contributing to gut problems, poor immunity, increased weight, insulin resistance, and sleep problems. Long-term unrelieved stress is linked to anxiety, depression, heart disease, and a higher risk of many chronic conditions.
Chronic stress activates the body’s “fight or flight” system, raising levels of stress hormones like cortisol and, over time, contributing to gut problems, poor immunity, increased weight, insulin resistance, and sleep problems. Long-term unrelieved stress is linked to anxiety, depression, heart disease, and a higher risk of many chronic conditions.
Evidence-based methods can calm the nervous system and protect both body and mind. These include meditation, deep breathing, yoga or tai chi, biofeedback, and structured programs such as Mindfulness-Based Stress Reduction (MBSR), which have been shown in studies to reduce stress and improve quality of life. Emerging research on the “gut–brain axis” suggests that eating a high-fiber, plant-predominant diet may support mental health by feeding beneficial gut bacteria, which in turn influence mood and inflammation.
Pillar 5 – Avoiding Risky Substances
![]() Tobacco, excessive alcohol, and misuse of other substances remain leading causes of preventable death and disability. In the United States, smoking is responsible for roughly 490,000 deaths per year, while alcohol contributes to about 178,000 deaths; drug overdoses are now among the leading causes of death for adults aged 18–44.
Tobacco, excessive alcohol, and misuse of other substances remain leading causes of preventable death and disability. In the United States, smoking is responsible for roughly 490,000 deaths per year, while alcohol contributes to about 178,000 deaths; drug overdoses are now among the leading causes of death for adults aged 18–44.
Reducing or quitting smoking and limiting alcohol use can dramatically improve heart and lung health, lower cancer risk, and improve mental well-being. Lifestyle Medicine clinicians often combine behavioral counseling, support groups, and—when appropriate—medications or nicotine replacement to help people succeed.
Avoiding risky substances is one of the most powerful longevity tools available.
Pillar 6 – Social Connections: The Healing Power of Relationships
![]() One of the longest-running scientific studies, the Harvard Study of Adult Development, has followed people for more than 80 years and found a consistent message: the quality of our relationships strongly predicts both happiness and health. People with strong, supportive relationships tend to have lower rates of depression, heart disease, and early death compared with those who are socially isolated.
One of the longest-running scientific studies, the Harvard Study of Adult Development, has followed people for more than 80 years and found a consistent message: the quality of our relationships strongly predicts both happiness and health. People with strong, supportive relationships tend to have lower rates of depression, heart disease, and early death compared with those who are socially isolated.
Social isolation has been linked to about a 50% increased risk of dementia, a 29% higher risk of heart disease, and a 32% higher risk of stroke. Group-based programs, community gatherings, volunteering, and faith or cultural communities can create a sense of belonging that supports both mental and physical health.
Loneliness is as harmful as many traditional medical risk factors—but building relationships is a powerful, enjoyable ‘treatment.’
Integrating Lifestyle and Traditional Medicine
![]() Lifestyle Medicine does not replace traditional or “allopathic” medicine; instead, it works alongside it. In emergencies—such as heart attacks, infections, trauma, or surgical problems—medications, procedures, and hospital care are essential and often lifesaving. However, for long-term conditions like high blood pressure, type 2 diabetes, high cholesterol, and obesity, daily habits heavily influence outcomes. When patients adopt healthier eating patterns, become more active, sleep better, manage stress, avoid risky substances, and strengthen social connections, many can prevent disease, reduce complications, and in some cases place disease into remission and reversal
Lifestyle Medicine does not replace traditional or “allopathic” medicine; instead, it works alongside it. In emergencies—such as heart attacks, infections, trauma, or surgical problems—medications, procedures, and hospital care are essential and often lifesaving. However, for long-term conditions like high blood pressure, type 2 diabetes, high cholesterol, and obesity, daily habits heavily influence outcomes. When patients adopt healthier eating patterns, become more active, sleep better, manage stress, avoid risky substances, and strengthen social connections, many can prevent disease, reduce complications, and in some cases place disease into remission and reversal
A Practical Prescription for Readers
A modern, realistic version of the ancient medical advice “Let food be thy medicine” might look like this: eat mostly plants, move your body every day, protect your sleep, calm your mind, avoid harmful substances, and stay closely connected to people who care about you. These are not quick fixes, but small, steady changes that add up over months and years to better energy, improved lab results, fewer medications, and a longer, healthier life.
To get started this week, readers can pick just one or two small steps—such as adding an extra serving of vegetables, walking 10–15 more minutes per day, setting a regular bedtime, or reconnecting with a friend—and build from there. When guided by a trained Lifestyle Medicine physician, these simple actions become part of a structured, evidence-based plan to prevent, treat, and in some cases reverse chronic disease.
Let me conclude with this quote
“The doctor of the future will give no medicine but will interest his patients in the care of the human frame, in diet, and in the cause and prevention of disease” – Thomas Edison
Key References for Further Reading
· Centers for Disease Control and Prevention – Chronic Disease Data and National Center for Chronic Disease Prevention (2024).
· American Heart Association and American College of Cardiology – Lifestyle and prevention guidelines.
· National Sleep Foundation – Adult sleep duration recommendations.
· Harvard Study of Adult Development – Long-term research on relationships and health.
· Harvard T.H. Chan School of Public Health – Ultra-processed foods and brain health (MIND diet and inflammation).
· Peer-reviewed lifestyle medicine and chronic disease remission reports, including intensive lifestyle interventions for type 2 diabetes.