Recent research suggests that certain medical routines, including screenings and medications, may be unnecessary for older adults, prompting a reevaluation of their benefits versus risks.
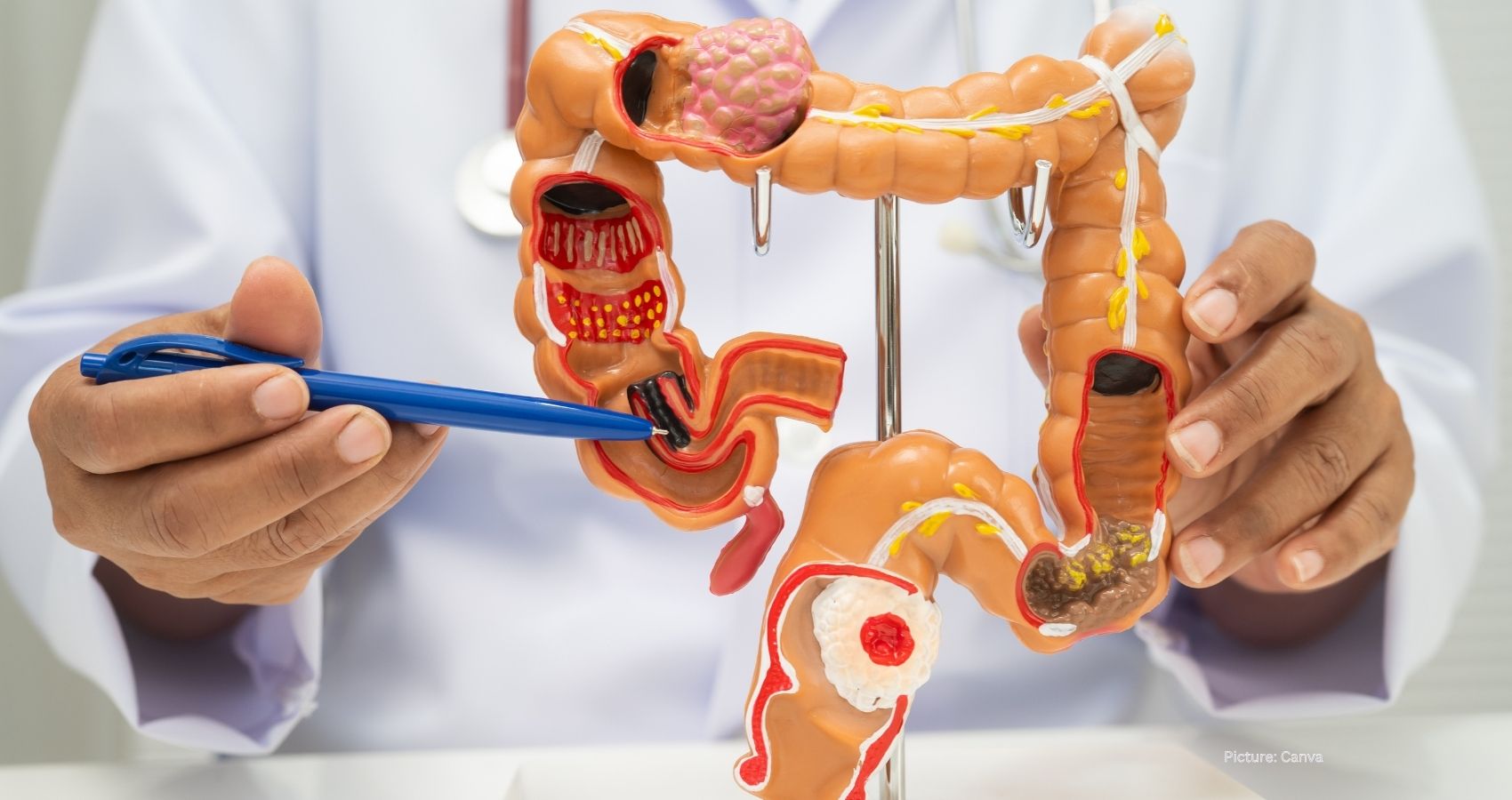
As medical practices evolve, healthcare providers are increasingly questioning the necessity of certain procedures and treatments for older patients. A recent case involving an 85-year-old woman highlights this trend, particularly regarding colonoscopies. Steven Itzkowitz, a gastroenterologist at the Icahn School of Medicine at Mount Sinai in New York, noted that while the patient met the criteria for a repeat colonoscopy, the risks associated with the procedure warranted a second look.
The patient was in reasonably good health, but the risks of undergoing a colonoscopy—such as bleeding, reactions to anesthesia, and potential perforation of the colon—were not insignificant. Moreover, the need to temporarily discontinue her blood thinners, due to cardiac stents, further complicated the decision. Itzkowitz reflected on how, just a few years ago, he would have scheduled the procedure without hesitation. However, emerging research indicates that the benefits of repeat colonoscopies diminish significantly after age 75.
This case is not isolated. Many healthcare professionals are reconsidering the risks and benefits of common screenings, procedures, and medications for older adults. Recent studies have raised questions about the necessity of removing certain skin lesions, the long-term use of thyroid medication, and the overall value of colonoscopies in this age group.
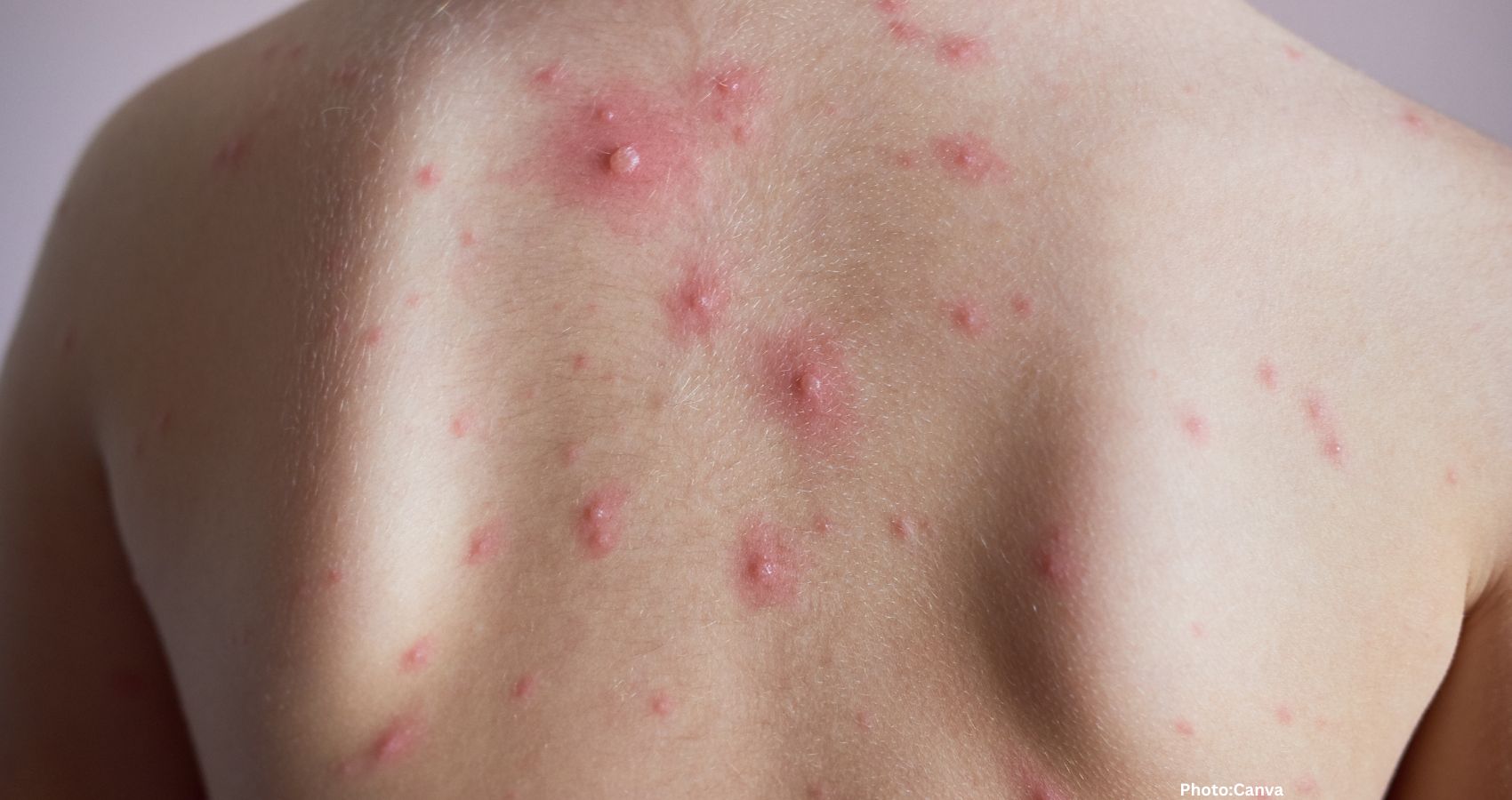
Actinic keratoses, or rough patches on the skin resulting from sun exposure, are commonly found in older adults. A study of Medicare beneficiaries revealed that nearly 30% were diagnosed with these lesions over five years. Traditionally, these patches are often removed through methods such as cryosurgery or laser therapy, based on the belief that they could progress to skin cancer. However, dermatologist Allison Billi from the University of Michigan points out that the likelihood of actinic keratoses becoming cancerous is less than 1 in 1,000 for patients without a history of skin cancer. Furthermore, treatment can be painful and may lead to complications like swelling and discoloration.
Billi advocates for a more conservative approach, suggesting that primary care doctors monitor these lesions annually for any concerning changes rather than resorting to immediate removal. She emphasizes that not every condition requires aggressive treatment, and simple preventive measures, such as using sunscreen, can be effective.
Another area of concern is the use of levothyroxine, a medication prescribed for hypothyroidism. Jacobijn Gussekloo, a primary care doctor and researcher at Leiden University Medical Center, explains that while many patients take levothyroxine for life, research indicates that older adults with subclinical hypothyroidism may not need to continue the medication indefinitely. Gussekloo’s team found that hormone levels often normalize on their own, and the medication may not provide significant benefits for this population.
Moreover, levothyroxine can interact with other medications and requires regular lab tests, leading to increased healthcare costs and potential side effects, such as hyperthyroidism. The Dutch researchers developed a protocol to gradually taper off the medication over 30 weeks, with ongoing monitoring. Remarkably, a quarter of participants aged over 60 were able to discontinue levothyroxine while maintaining healthy thyroid function.
However, healthcare professionals caution against abrupt discontinuation of the medication without medical supervision. Maria Papaleontiou, an endocrinologist at the University of Michigan, emphasizes the importance of careful monitoring and individualized treatment plans, noting that some patients will always require levothyroxine.
The question of when to stop screening for colon cancer is another contentious topic. The U.S. Preventive Services Task Force has assigned a lukewarm C rating to colonoscopies for individuals over 76, citing minimal benefits. Despite this, a recent study found that nearly 60% of older patients with limited life expectancy were still advised to undergo screening. Samir Gupta, a gastroenterologist at the University of California-San Diego, frequently encounters patients who are at low risk for colon cancer but are still subjected to the risks of the procedure.
Gupta’s research involving nearly 92,000 Veterans Affairs patients over 75 revealed that while a small percentage developed adenomas—polyps that can become cancerous—only a fraction died from colon cancer. In fact, the majority of patients in the study died from other causes, underscoring the limited impact of colonoscopies on longevity.
Despite the evidence, many patients who have had polyps removed express a desire to continue with regular colonoscopies. Shifting established medical norms can be challenging, as both patients and healthcare professionals may resist changes to longstanding practices. This resistance is also evident in other areas, such as mammograms for older women and prostate cancer screenings for older men.
Ultimately, the decision to undergo medical procedures or continue medications should be individualized, taking into account the patient’s overall health, preferences, and life expectancy. Itzkowitz concluded his conversation with the 85-year-old patient by suggesting she could forgo another colonoscopy, a recommendation that seemed to please her.
As the medical community continues to explore the complexities of care for older adults, it is crucial to balance the potential benefits of interventions with the associated risks, ensuring that patients receive the most appropriate and effective care.
According to KFF Health News, the ongoing dialogue surrounding these medical routines reflects a broader trend toward personalized healthcare for older adults.